Strabismus Explained
Strabismus refers to a fairly common visual disorder in which there is some degree of eye misalignment. There are many different forms of strabismus, but all of these disorders involve one eye that’s not able to clearly focus on an object. Although strabismus can affect anyone at any age, it’s most often seen in infants and young children.
All parents need to be aware of strabismus’s warning signs and constantly monitor their child’s eyes for symptoms. Without early intervention, children with strabismus are more at risk for visual complications and psychological issues like depression.
Below, we’ll explore what strabismus is, how it’s caused, and the treatments available to patients.
What Are The Major Forms Of Strabismus?
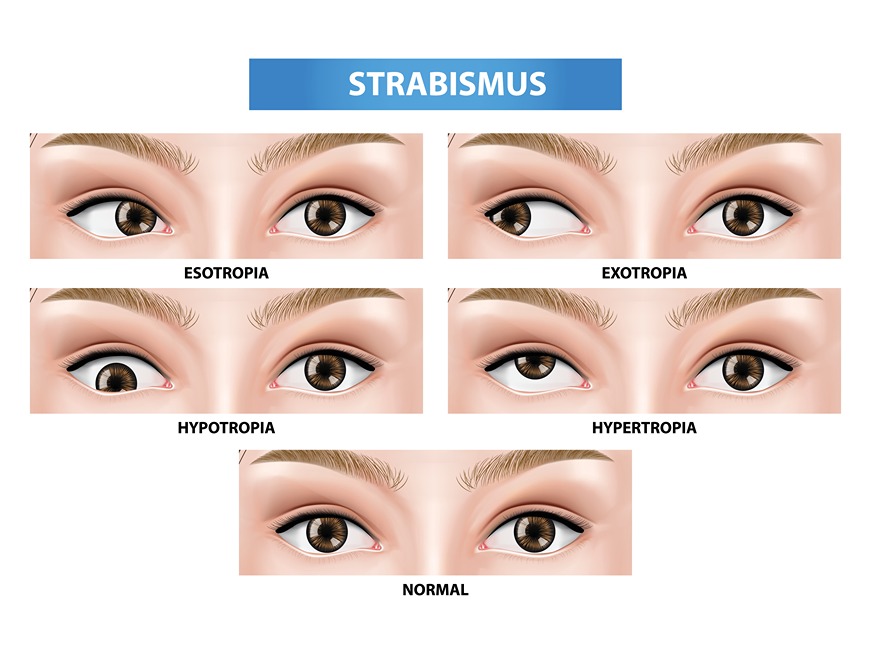
Instead of one “standard strabismus,” there are dozens of potential vision problems that could fall under this medical term. Major variants of strabismus include esotropia, exotropia, hypertropia, and hypotropia. In each of these disorders, the misaligned eye tends to look in a different direction.
Of these four, esotropia is the best known. You’ve probably already heard of this disorder by its nickname “cross-eyed.” As the name suggests, patients with crossed eyes have one eye with a pupil that points toward the nose.
Exotropia is exactly the opposite of esotropia. People who have this disorder have one pupil that points out towards the temple.
Similar to esotropia and exotropia, hypertropia and hypotropia are opposites in vertical directions. Hypertropic patients have one eye that points up, whereas hypotropics have one eye that looks down.
Strabismus is further complicated by yet another division: constant versus intermittent. As you might’ve guessed from the terms, patients with constant strabismus have similar symptoms all the time, while intermittent patients have symptoms that come and go.
Interestingly, there are some strabismus patients that sometimes have a misaligned right eye and then have a misaligned left eye. Most strabismus sufferers, however, only have one eye that’s always out of alignment.
According to the NHS, it’s common for children to have intermittent strabismus before they turn three months old. If these intermittent symptoms persist after a child turns three months, however, parents should bring them to an optometrist for a check-up.
Early Warning Signs And Symptoms Of Strabismus
Most often you could easily detect whether or not a child has strabismus by looking at his/her eyes. If you see the child’s pupils are misaligned when you’re talking to them, then they have some form of this disorder.
Besides misalignment in the pupils, children with strabismus will often tilt their heads to help them get a clearer focus on an object. These patients might also experience blurred vision, double vision, frequent headaches, and eye pain.
Potential Causes Of Strabismus
Just as there’s not a single form of strabismus, so too there’s no one cause of this disorder. Indeed, there are many potential causes of this disorder that range wildly in terms of severity.
Most often strabismus is the result of poor communication between the brain and eye muscles. Sometimes an eye will become misaligned to overcompensate for an underlying vision problem like myopia or astigmatism.
There are a few doctors who have suggested strabismus may have a genetic component, although more research is needed to establish this link. As a precaution, families that have a history of this disorder should be on high alert for strabismus warning signs in newborns.
In more serious cases, strabismus could be caused by certain infections or neurological conditions. For instance, autistic children have a higher chance of developing strabismus than non-autistic children. Patients who’ve suffered direct trauma to the eyes or a stroke could also develop strabismus.
Other potential reasons for strabismus include measles, Down’s syndrome, or cerebral palsy. Although extremely rare, strabismus could also be an early warning sign of eye cancer.
Will Strabismus Go Away On Its Own?
Unlike other “growing pains,” strabismus doesn’t go away with age. In fact, this disorder gets worse the longer parents wait to bring their child in for treatment.
Children who don’t get early treatment for strabismus will develop amblyopia in their weaker eye. Most often called “lazy eye,” amblyopia occurs because the brain favours the more dominant eye at the expense of the misaligned eye. Once amblyopia sets in, it becomes more difficult to restore the neural pathways connecting the misaligned eye to the visual cortex.
It’s not impossible to correct amblyopia in its early stages, but it’s far more difficult than addressing strabismus. If amblyopia develops without any treatment, however, then a child could lose their sight in one eye.
Studies have also shown that patients with unaddressed strabismus are more at risk of other visual and even psychological issues. Doctors now say that patients with strabismus are far more likely to develop myopia than children without the visual disorder. Children who have strabismus also tend to have a higher tendency to develop ADD or ADHD, which leads to poor academic performance.
Treatments For Strabismus
The treatment methods optometrists use to combat strabismus largely depend on the cause and severity of the patient’s issue. Some patients might only require prescription eyeglasses or contact lenses, but others might need intensive training and/or surgery.
Before discussing what strabismus surgery might entail, let’s detail a few of the more common strabismus exercises patients can practice at home.
Two Common Strabismus Exercises
In most cases of strabismus, eye exercises are essential to help realign the eyes. Optometrists will teach their patients the exact eye movements they need to master at home, and recommend how many times patients should repeat these exercises per day.
It’s critical that the patient and their parents understand how to perform each exercise thoroughly before leaving the doctor’s office. For optimal success, parents should monitor their child’s progress and encourage them to get into a regular routine.
One example of a common strabismus exercise is the “pencil pushup.” To start this exercise, find a pencil and hold it at eye level with the eraser facing you. Now, extend the hand holding the pencil one arm’s length away. Focus all of your attention on the eraser as you gradually bring the pencil towards your face. Once the eraser becomes blurry, start over again and repeat a few times. Over time, this exercise will help improve eye coordination.
Another popular strabismus exercise is known as the Brock String method, which was named after the ophthalmologist Frederick W. Brock. For this exercise, get a piece of white string between 5 to 10 feet long and place three different coloured beads about 20 cm apart from each other on the string. One end of this string should be secured on a non-moving object (e.g. a door handle) and the patient should hold the other end by his/her nose. Before beginning the exercise, ensure the string is taut and pointed downwards slightly.
Once everything is set up, the patient should stare for a few seconds at each bead starting in the middle and moving closer. The bead that’s being focused on should look clear and single, but the other beads should appear double. Also, the string should appear to form an X-pattern with the middle point at whatever bead you’re focusing on.
Once a child is able to see these three patterns clearly, you can increase the difficulty of this test by slowly pushing the closest bead toward the patient’s nose. If the child starts to see this bead as double, then they must push the bead back until there’s only one. After the closest bead is properly adjusted, look at the furthest bead and then the middle bead.
Benefits Of Patching Therapy
In addition to these exercises, optometrists might advise strabismus patients to place an eye patch over their dominant eye. Patching is one of the most effective ways to naturally re-train a child’s weaker eye.
If a child doesn’t like patching for some reason, it’s possible to use atropine drops instead of an eye patch. Placing a few atropine drops in the child’s dominant eye will blur vision temporarily, forcing the brain to make connections with the weaker eye. Parents could discuss atropine drop therapy with their optometrist if they’re struggling with regular patching therapy.
How long a patient needs to wear an eye patch will be assessed and reviewed by an optometrist. Sometimes children have to wear these eye patches all day, while others could wear them for just a few hours. Patching therapy could last a few months or a few years. Patients should only remove eye patches once their optometrist says it’s safe to do so.
Surgical Options For Strabismus
For a more serious case of strabismus, an optometrist might recommend either Botox injections or surgery. In both cases, the goal of these procedures is to balance out the patient’s eye muscles.
If one muscle is too strong, for example, the surgeon will try to weaken it by cutting and re-attaching the offending muscle further back in the patient’s eye. Botox injections directly into the eye also help to relax muscles that are too strong.
After the surgery is completed, some patients experience severe eye redness and might feel something “stuck” in their eyes. Usually, these symptoms are nothing to worry about and they will clear away within a few weeks. Although not impossible, it’s rare for patients who undergo strabismus surgery to experience complications like eye infections or permanent scarring.
Early Treatment Is Critical For Strabismus Success
Data from London’s Moorfields Eye Hospital estimates that one in 20 children in the UK has some form of strabismus. Thankfully, this disorder can be easily corrected if parents bring their child to an optometrist in the early stages. Without proper care early on, however, strabismus will develop into more serious eye conditions like amblyopia. Parents shouldn’t wait to bring their child in for a visual screening if they notice the warning signs of strabismus.